Varicose Veins: Causes and Risk Factors
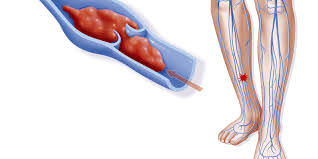
For many who suffer from them, varicose veins are a cosmetic annoyance. These red, blue, or purple vessels have a ropelike appearance and most often occur on the legs. For some patients, they create discomfort and the possibility of complications such as deep vein thrombosis. Understanding what causes these abnormal blood vessels and the risk factors for developing them can help patients make the best treatment decisions for regaining their active lives.
What Causes Varicose Veins?
Blood vessels become varicose because of venous insufficiency. Johns Hopkins Medicine notes that the function of one-way valves in veins is to transport blood from extremities to the heart. However, if valves have become damaged or weakened, they permit blood to fall backward and collect behind them. When patients stand or sit for extended amounts of time, blood pools in a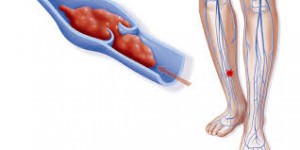 vein. This exerts pressure on the vessel and can cause it to stretch, sometimes resulting in a varicose vein. Eventually, the individual might experience swelling, pain, throbbing, aching, or burning in addition to discolored blood vessels. Some varicose vein patients find it difficult to sleep because they develop restless leg syndrome.
vein. This exerts pressure on the vessel and can cause it to stretch, sometimes resulting in a varicose vein. Eventually, the individual might experience swelling, pain, throbbing, aching, or burning in addition to discolored blood vessels. Some varicose vein patients find it difficult to sleep because they develop restless leg syndrome.
What Are the Most Common Risk Factors?
Nothing can guarantee that a patient will never develop these abnormal veins. However, understanding the risk factors for this disorder can alert individuals with above-average risk of the need to consult with a vein specialist. According to the National Heart, Lung, and Blood Institute, a number of factors increase the possibility of a varicose vein. The most common include:- Genetics. Around 50 percent of varicose vein patients have family members who have had this disorder.
- Aging. The aging process weakens veins, causing them to work less efficiently.
- Female gender. Women have a much greater risk for varicose vessels than men do. This is due to hormonal fluctuations throughout a woman’s life.
- Pregnancy. Pressure from a developing fetus can cause varicose vessels that usually improve after delivery.
- Extra pounds. Being obese or even overweight causes additional pressure on veins.
- Remaining stationary. When individuals stand or sit for prolonged periods, inactivity can force greater vascular exertion to transport blood upward.
- Limb trauma. Injury from trauma or prior blood clots can weaken vein valves.
- Increasing exercise to boost circulation in the extremities
- Losing excess pounds and eating a diet low in salt
- Elevating the legs periodically to improve circulation
- Standing and sitting for shorter periods
- Avoiding crossed legs when seated




